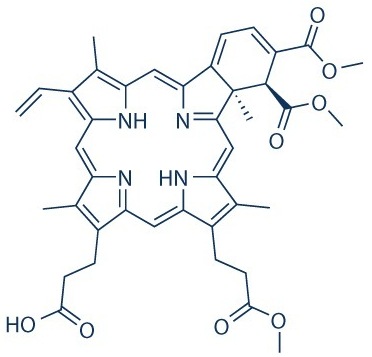
Overview of Verteporfin
Verteporfin is an FDA approved medication used in the treatment of age-related macular degeneration. It is also used off label for central serous retinopathy. For the treatment of these conditions, the drug is photo-activated using red light. In its non-photoactivated form, it is an inhibitor of the Yes-associated protein (YAP) (Mascharak et al 2021). YAP has been implicated as one of the primary drivers of the signaling cascade which leads to the generation of scarring fibroblasts in humans (Parry and Allison 2022). In their embryonic period, animals such as mice, pigs and humans have a unique ability to regenerate damaged tissues (Parry and Allison 2022). This ability is lost in humans in the third trimester and in mice at approximately postnatal day 17 (Clark 2021). Scar tissue lacks the strength and elasticity of unwounded tissue, as well as secondary appendages such as hair follicles and sweat glands. YAP inhibition has been proven in mice (Mascharak et al 2021) and in pigs (Longaker et al 2022) to inhibit scar tissue formation and promote the regeneration of tissue with non-fibrotic extracellular matrix (ECM) structure and normally functioning secondary dermal appendages like hair follicles and sweat glands. It has also been shown to work in human lung tissue. This regenerative ability, therefore, lies latent, despite the postnatal transition to scar tissue formation as the default evolutionary pathway of wound healing.
Detailed Summary of Verteporfin and Scar Tissue Etiology
A dichotomy exists wherein reticular dermal fibroblasts may express Engrailed-1 (En1) and assume either En1-negative fibroblast (ENF) or En1-positive fibroblast (EPF) lineages. As outlined in Parry and Allison’s review on wound healing, after injury, dermal fibroblasts may activate En1 to become EPFs and contribute to formation of scar tissue. The bifurcation of these dermal fibroblast lineages is regulated by their inherent mechanoresponsiveness. Upon injury, dermal fibroblasts are able to sense mechanical strain via its transduction into a biochemical signal. This strain occurs between a network of cell-ECM interfaces called focal adhesions (FA) (Provenzano and Keely). The mechanotransduction occurring at these interfaces results in the phosphorylation of focal adhesion kinase (FAK), a regulator of FA signaling, resulting in the downstream expression of the Yes-associated protein (YAP). YAP acts as a biomolecular strain status signal, indicating whether fibroblasts are under tension or experiencing mechanical strain, even in unwounded tissue. YAP initiates the signaling cascade which causes ENFs to express En1 and become EPFs, leading to pro-fibrotic tissue development.
By interrupting signaling with the YAP inhibitor, Verteporfin, fibroblasts never receive the signal indicating that tissue is experiencing mechanical strain and, when they are recruited in tissue remodeling, they remain ENFs rather than expressing En1 and becoming pro-fibrotic EPFs. Thus, tissue remodeling occurs with the generation of normally functioning hair follicles, sweat glands, ECM ultrastructure and the mechanical strength and elasticity of unwounded skin.
Why has Dr Barghouthi Chosen to Research Verteporfin?
Verteporfin has the potential to improve wound healing in any surgery, in Dr Barghouthi’s case he is interested in verteporfin’s potential to improve the outcomes of hair transplant surgery. Find out more about the potential benefits of verteporfin.
Support
While Dr. Barghouthi has a responsibility to his patients in maintaining his clinical practice, he is dedicated to pursuing research in hair loss. His responsibilities limit the time available for research days and associated costs. Financial support will help accelerate research of hair restoration and scarless wound healing so that Dr. Barghouthi and his team can recruit and sponsor more patients and free up more clinic time for research. Future plans are in order to test Verteporfin further with varying doses, methods of administration, and with a FUT candidate in addition to his initial tests with FUE candidates. Each experiment varies between roughly 12,500 USD – 15,000 USD. This accounts for medication and equipment, staff operative costs, follow ups, and use of dermoscopy. Financial incentives are also offered to volunteers in return for their cooperation. Your support is wholeheartedly appreciated.
CORRESPONDENCE
Dr. Barghouthi would like to extend communication to other doctors interested in protocol development, sharing of data, and discussion of parallel execution of a test protocol matrix.
If you are interested in collaborating, please contact Dr. Barghouthi